Menopausal Problems, Pelvic Pain, Hot Flushes, Urinary Incontinence, and any other complaints.

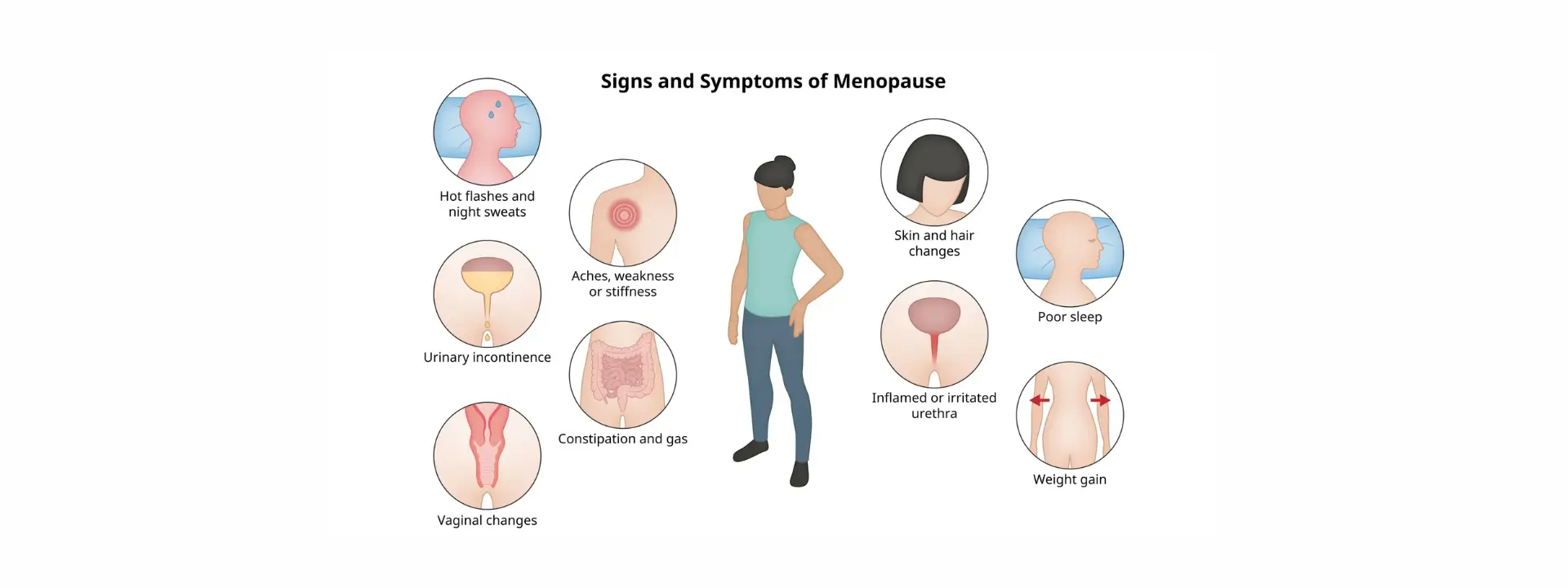

Menopausal Problems, Pelvic Pain, Hot Flushes, Urinary Incontinence, and any other complaints.
Experience superior Menopause care at RoyalDocline. With 30 years of expertise, our OBGYN service provides personalized treatments, routine check-ups, and specialized support for menopause. Prioritize your health—book an appointment today.
Menopausal problems, pelvic pain, hot flushes, and urinary incontinence are common issues that women may face during and after menopause. Proper evaluation and treatment can significantly improve the quality of life for women experiencing these symptoms. Here’s an overview of evaluation and treatment options:
Evaluation:
Medical History:
- Detailed information about menopausal symptoms, pelvic pain, and urinary incontinence.
- Any relevant medical history, including surgeries, gynecological conditions, and medications.
Physical Examination:
- Pelvic examination to assess the health of reproductive organs.
- Evaluation for signs of pelvic floor dysfunction.
Diagnostic Tests:
- Blood tests to measure hormone levels, including estrogen and follicle-stimulating hormone (FSH).
- Imaging studies, such as ultrasound or MRI, to examine pelvic organs and rule out structural abnormalities.
Bladder Function Tests:
- If urinary incontinence is a concern, urodynamic testing may be done to assess bladder function.
Bone Density Test:
- Assessing bone density to evaluate the risk of osteoporosis, a common concern in menopausal women.
Treatment:
Hormone Replacement Therapy (HRT):
- HRT can alleviate menopausal symptoms such as hot flushes and vaginal dryness by supplementing estrogen and, if necessary, progesterone. However, the decision to use HRT should be individualized and made in consultation with a healthcare provider due to potential risks and benefits.
Non-Hormonal Medications:
- Certain medications, such as selective serotonin reuptake inhibitors (SSRIs) or selective norepinephrine reuptake inhibitors (SNRIs), may be prescribed to manage hot flushes.
Pelvic Pain Management:
- Physical Therapy:
- Pelvic floor physical therapy can help address pelvic pain and improve muscle function.
- Medications:
- Pain medications, muscle relaxants, or nerve medications may be prescribed based on the underlying cause of pelvic pain.
- Physical Therapy:
Urinary Incontinence Treatment:
- Pelvic Floor Exercises (Kegel Exercises):
- Strengthening pelvic floor muscles can improve urinary incontinence.
- Behavioral Therapies:
- Bladder training and biofeedback may be used to manage incontinence.
- Medications:
- Certain medications can help control overactive bladder or stress incontinence.
- Surgical Options:
- In some cases, surgical procedures like sling placement may be considered for urinary incontinence.
- Pelvic Floor Exercises (Kegel Exercises):
Lifestyle Modifications:
- Healthy lifestyle habits, including a balanced diet, regular exercise, and adequate hydration, can contribute to overall well-being during menopause.
Alternative Therapies:
- Some women find relief from symptoms through complementary approaches like acupuncture, yoga, or herbal supplements. However, the evidence for these interventions varies, and it’s crucial to consult with a healthcare provider before trying them.